First, the good news. Thanks to the Affordable Care Act and regulatory changes made in recent years by the Internal Revenue Service, a greater wealth of information is available to the public than ever before about how nonprofit hospitals are meeting their obligations to the communities surrounding them.
Now, the bad: You need the digging skills of an investigative journalist, the know-how of a statistician and a background in hospital management to make heads or tails of that data.
“There has been a lot of progress made in improving transparency. Unfortunately, it is still not very consumer-friendly,” said Adela Flores-Brennan, executive director of the Colorado Consumer Health Initiative. “It is challenging and time-consuming to track down all of the information that would give a comprehensive picture of community benefits.”
The underlying idea behind disclosure is that because nonprofit hospitals enjoy enormous benefits from the public, they are both obligated to serve the public – that’s the community benefit part – and to be transparent about how they are doing it. The value of the tax exemptions that the nation’s 2,900 public hospitals enjoy is enormous: an estimated $8.5 billion to $21 billion, according to the Hilltop Institute at the University of Maryland, Baltimore County. The Joint Committee on Taxation estimated such benefits to be $12.6 billion in 2002.
Thirty-one states require some sort of reporting of community benefits by nonprofit hospitals to state agencies; Colorado is not one of them, according to data gathered by the Hilltop Institute.
However, Colorado nonprofit hospitals must meet federal reporting requirements. Since 2009, following congressional hearings that highlighted problems and abuses, the IRS has required nonprofit hospitals to report the “community benefits” they provide. These are divided into six broad categories, ranging from amount spent on uncompensated care to training for medical students to the somewhat amorphous category of “community health improvement.”
The ACA added some new requirements. In 2012 nonprofit hospitals became obligated to conduct community health needs assessments every three years. And they must produce written financial assistance policies along with plans to publicize those policies in the communities they serve. Both of these documents must be made “widely available” on a website. The IRS only issued final rules on these requirements in December 2014, nearly five years after passage of the ACA.
Understanding the Numbers
Finding all this information, however, is not only a chore, it’s difficult for a layperson to interpret. Nonprofit hospitals report their spending on different categories of community benefits on a tax form known as Schedule H, which is appended to the 990s they file as charitable organizations, which often run more than 100 pages. Hospitals file these forms at the system level, not by individual hospital.
While a community member may ask a hospital to produce these 990s, they are also accessible through online search sites such as the Foundation Center and GuideStar. So, for example, it’s possible to see that Children’s Hospital Colorado, on the high end, reported spending 21.3 percent of its total expenses on community benefits in 2013, while Portercare Adventist Health System reported spending 5.9 percent.
One big wrinkle: Government-run hospitals, such as Denver Health and the University of Colorado hospitals, are not required to file 990s and the Schedule H forms.
Furthermore, these figures can be misleading, caution experts. First, sometimes there are discrepancies between what hospitals report in a given community benefit category and what they report about their financial status elsewhere on the 990 form. In a comprehensive analysis of community benefits reported by nonprofit hospitals in 2009, published in the New England Journal of Medicine in 2013, researchers found such errors, although they were able to correct them with some digging from other data sources.
Another problem might be underreporting in some categories. Because the IRS has left gray what can be counted in the “community health improvement” category, hospitals may not include all the activities that they do for fear that the IRS won’t allow it. Increasingly, hospital systems are defining health broadly and may get involved in issues not traditionally thought of in the health care category.
In April, the American Hospital Association and the Catholic Health Association of the United States, seeking some clarity, wrote the IRS requesting that the agency “formally acknowledge that support for improved housing to enhance the health of a hospital’s community is a community benefit and should be recognized on ... Schedule H."
Key Transparency Requirements for Hospitals
- All nonprofit hospitals are required to report community benefits to the IRS on Schedule H of 990 tax forms. These are filed annually.
- In addition, the ACA requires nonprofit hospitals to conduct Community Health Needs Assessments (CHNAs) and financial assistance policies and make them “widely available” on a website.
- Government hospitals are not required to file 990 tax forms. However, they are required to conduct CHNAs and post financial assistance policies.
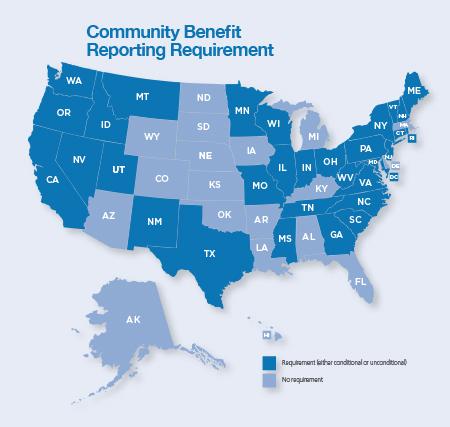
- The state of Colorado has no separate requirements for nonprofit hospitals to report community benefits, nor do 18 other states as shown in map below. At least one national study showed that nonprofits in states with a local reporting requirement – in addition to the federal rules – tend to spend more on community benefits.
- However, a 2012 Colorado law, the Hospital Payment Assistance Program, and 2014 follow-up legislation, do establish requirements for financial assistance and require both private and nonprofit hospitals to publicize these policies in the communities.
Charity Care Reporting
Meanwhile, community benefit reporting rules need to catch up with the new landscape after passage of the ACA. The percentage of uncompensated care provided, or charity care, is typically the largest that nonprofit hospitals report. For example, among five Colorado nonprofit hospital systems, the charity care percentage reported ranged from 7.58 to 15.33 percent. In the other categories, the reported percentages were all 1 percent or lower.
However, charity care levels “tell us more about the neighborhoods being serviced by the hospital” than a full picture of community benefits, said Phillip Gonzalez, program director of Community Catalyst, a national consumer health nonprofit organization.
In addition, in states such as Colorado, which implemented Medicaid expansion following passage of the ACA, hospitals are reporting lower charity care levels as people gain insurance. Nationwide, states that expanded their Medicaid programs saw a 29 percent increase in participation, a 30 percent decrease in charity care patients and a 25 percent decrease in self-pay patients, according to a Colorado Hospital Association analysis of 2014 first quarter data.
In this new world, it’s important to watch a growing category of people: the underinsured, said Gonzalez. “What does it matter if you have coverage but your deductible is $10,000 or $15,000? Are you going to behave as if you are insured or uninsured?”
Beyond the reporting of community benefits on Schedule H, consumers can also look at the community health needs assessments conducted by hospitals. For example, Children’s Hospital Colorado makes available online its 2012 analysis of community health needs. The survey identified four areas as priorities: access to health care, obesity, injuries and mental health.
Evaluating how well a given hospital system has conducted its community health needs assessments, however, is somewhat subjective since they all follow different formats; it is not a simple number that can be put in a spreadsheet. Community Catalyst recommends looking at who was involved in the assessment, who was left out and who should be included; how data were gathered and presented to the community; and the program’s impact.
As for new financial assistance policies required by the ACA – due by the end of this year – there may be some overlap with the Hospital Payment Assistance Program. Approved by the Colorado Legislature in 2012, this new law requires hospitals to create and publicize financial assistance policies. It also limits charges for certain patients – uninsured Coloradans making under a certain income level – to that of an insured patient. A 2014 law, S.B. 14-50, set up a committee of consumer and hospital representatives to clarify how the law should be enforced.
Hospitals recognize that providing the public information with the community benefits they offer is not only a requirement, but an important tool for gaining support. In September, the CHA launched its first survey of state hospitals – private and nonprofit alike – to gather not just information, but stories about community benefits programs. However, the association did not receive as much participation as it would have liked and so hopes to expand the project in this coming year, said Kevin Downey, vice president of communications and media relations at the CHA.
Unfortunately, while more information is available than ever before about hospital community benefits, it is far from complete. And gathering and interpreting it remain largely the province of experts.
This article was originally published in the Summer 2015 issue of Health Elevations.
